-

Jay
New Nutritional Products from Klaire Labs®
Mathews Chiropractic is extremely excited and pleased to announce we…
-

Caitlin Clark
Introducing Cold Laser Therapy
Mathews Chiropractic wishes you and your loved ones a bright…
-
Jay
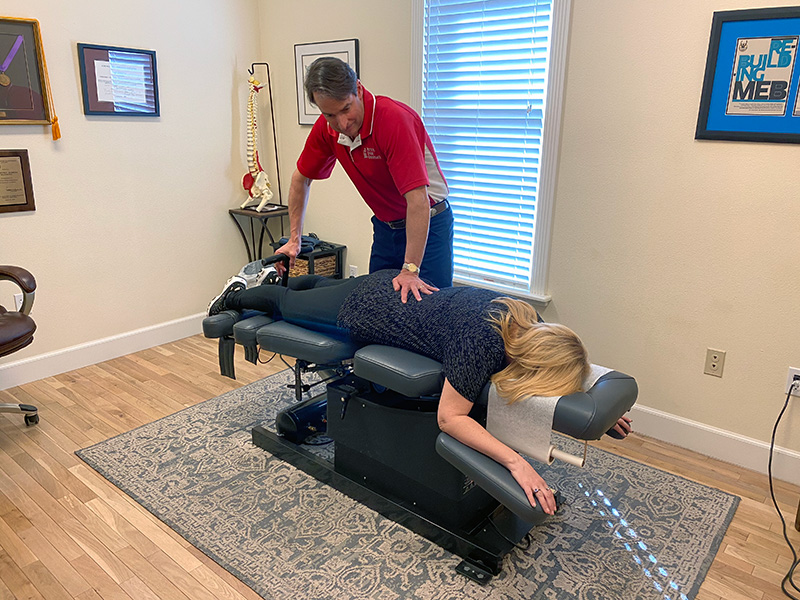
Hill Air-Flexion and Distraction Table
We are excited to announce that the new Hill Air-Flexion…
-

Jay
Maintain Your Movement and Avoid Arthritis!
Maintaining movement and range of motion in all of our…
-

-

Jay
Increase Your Mobility and Put the Brakes on OA
Increasing mobility can put the brakes on this degeneration. There…






